
Nuclear medicine is a medical imaging specialty that uses radiopharmaceuticals for diagnosis, staging of a disease, therapy and monitoring the response of a disease process. Depending on the type of the requested examination, the used radiopharmaceutical can be given to the patient via intravenous injection, orally or breathed in (inhaled).
The imaging modalities in nuclear medicine does not generate radiation. They only record the radiation emitted from the radiopharmaceutical inside the patient. In addition, nuclear medicine scans differ from radiology, as the emphasis is not on imaging anatomy, but on the function. For such reason, it is called a physiological imaging modality.
❰❰ IMAGING MODALITIES
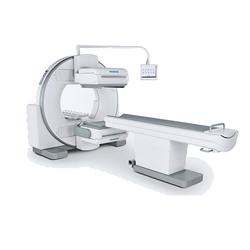
Single Photon Emission Computed Tomography (SPECT)

Positron Emission Tomography (PET)
❰❰ HYBRID MODALITIES
Nuclear medicine images can be fused using software or hybrid cameras, on images from modalities such as CT or MRI to locate the part of the body in which the radiopharmaceutical is concentrated.

❰❰ MAIN CATEGORIES
❰❰ HISTORY
Its started with the discovery of mysterious “rays” from uranium in 1896 by the French physicist Henri Becquerel following Wilhelm Conrad Roentgen’s discovery of x-rays in 1895. One year later, Marie Curie named the mysterious rays “radioactivity”. In 1903, Alexander Graham Bell suggested that these radioactive waves could have a role in medicine by placing a sources containing radium in or near tumors.

Wilhelm Röntgen
1845 – 1923

Antoine Henri Becquerel
1852 – 1908

Marie Curie
1867 – 1934
First paper about the use of radium for therapy was published in 1913, by Frederick Proescher and the first clinical therapeutic application was on 1936, by John H. Lawrence when he used phosphorus-32 to treat leukemia.
The discovery of the most important radionuclide in nuclear medicine (technetium-99m) was on 1938. However, because of the technical limitations at that time, advancements were slower before the making of short-lived radionuclide portable generators on 1957. One year later came the invention of the first scintillation camera (Gamma Camera) by Hal Anger and a few years later commercial gamma camera was released. Nuclear medicine kept evolving over the years. Now, nuclear medicine has evolved and fused with Computed Tomography and Magnetic Resonance Imaging producing top-shelf functional and morphological studies.
❰❰ RADIATION SAFETY
Nuclear medicine diagnostic procedures are safe except for pregnant ladies, unless it is requested by the physician for exceptional cases. However, the procedure better to be discussed with the doctor to know the desired benefits of the test and the alternative procedures, or you can ask the the nuclear medicine specialist about the procedure.
No, you shouldn’t because nuclear medicine scans use high-energy radioisotopes, the radiation passes directly from the other person without interacting with tissues. In contrast, wearing a lead apron slows down the radiation beam, which allows it to deposit its energy in the body and interact with tissues.
The risks from diagnostic doses are usually small compared to other lifetime risks to which the patient is exposed to and the amount of radiation dose in most diagnostic procedures is less than an x-ray, CT scan, or fluoroscopy.
When the body is exposed to radiation, tissue damage may occur, which in turn may damage DNA or chromosomes, increasing the risk of genetic mutations. When a fetus is exposed to radiation doses, it may cause abnormalities in an organ or irreparable damage and if the radiation dose is too high, it may cause the death of the fetus.
The radioactive dose used in diagnostic procedures in nuclear medicine is very low, unlike radiation treatments in which the amount of radioactive dose is high and this gives the desired effect on the tissues or organs when radiotherapy. That is why the patient must undergo a pregnancy test in the event of suspicion or if the pregnancy is uncertain before starting the therapeutic doses.
In diagnostic procedures the radioactivity is very low. However, the patient may be asked to maintain a distance of approximately one meter between him and his family members for a period of time given by the nuclear medicine specialist to protect them from exposure to radiation.
One the other hand, in therapeutic procedures, the patients may present some slight risk to their family members if they do not follow the INSTRUCTIONS ON RADIATION SAFETY given to them by the nuclear medicine specialist.



Leave a Reply